White Discharge (Vaginal Discharge) (Leucorrhea): Causes, Symptoms and Treatment
Is White Discharge Normal?
You’re not alone
White discharge, also known as vaginal discharge, is a common concern among women and can be normal or a sign of infection depending on the symptoms.
BV affects somewhere between 40% and 50% of women. Yeast infections are so common that most women will have at least one. Trichomoniasis, less talked about, is still one of the most common curable STIs. If you’ve noticed a white discharge problem, smelly discharge, or white discharge with itching, you are in very large company.
These changes fall under the umbrella term vaginitis. Which type matters, because the three main causes are completely different things that need completely different treatments. Getting this wrong wastes time and sometimes makes things worse. White discharge may sometimes be linked to hormonal conditions such as PCOS, or hormonal changes during adolescence or menopause.

Is White Discharge Normal?
A healthy vaginal environment is acidic, with a pH between 3.8 and 4.5. That acidity is the body’s defense system, maintained mainly by Lactobacillus bacteria, which produce lactic acid and crowd out harmful organisms.
Something that rarely gets mentioned: between 7% and 72% of women fall into “intermediate flora” — not a full infection, but not in balance either. If something feels off and your tests come back negative, this is often why. It’s real, and it doesn’t mean you’re imagining it.
Causes of White Discharge in Women
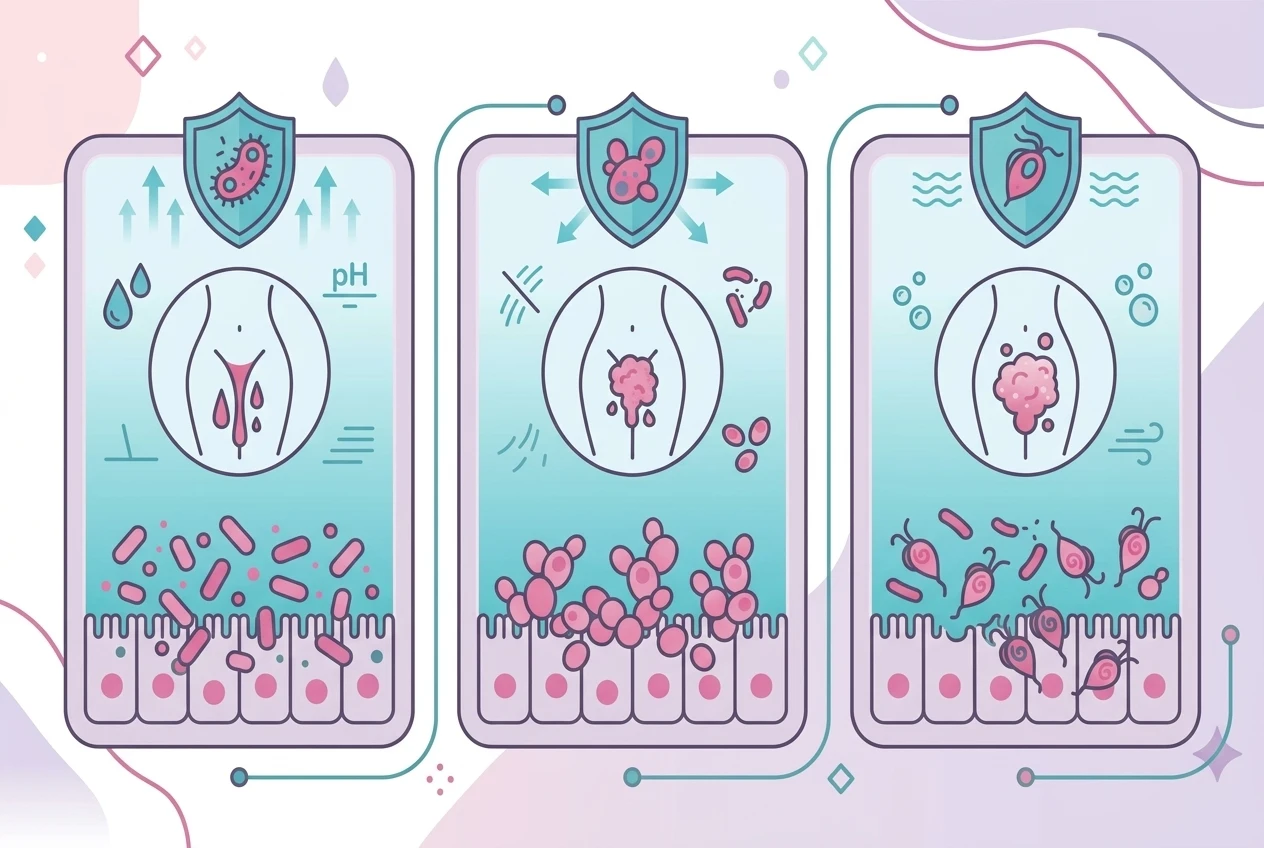
| Condition | What causes it | Discharge | Smell | Other signs |
|---|---|---|---|---|
| Bacterial Vaginosis (BV) | Overgrowth of anaerobic bacteria (Gardnerella, Prevotella, Mycoplasma, Mobiluncus, Ureaplasma) | Thin, off-white, sticks to vaginal walls | Fishy, often worse after sex | Usually no inflammation; pH above 4.5 |
| Yeast (Vulvovaginal Candidiasis) | Candida albicans | Thick, white, cottage-cheese texture | None | Intense itching, redness, burning; pH below 4.5 |
| Trichomoniasis | Trichomonas vaginalis (a parasite) | Greenish-yellow, frothy | Foul | Soreness, pain, inflammation; pH above 4.5 |
Types of Discharge and What They Mean
The colour and texture of your discharge often points to the cause. White, thick discharge that looks like cottage cheese is usually a fungal (yeast) infection. Yellow or greenish discharge, especially if frothy, is more likely to be an infection like BV or trichomoniasis. Foul-smelling discharge, particularly with a fishy odour that gets worse after sex, is a strong sign of bacterial vaginosis.
Clear or slightly white discharge that changes across your cycle is normal and not a reason to worry. The key is whether something has changed from what is usual for you.
Noticed a change in your discharge? A quick consultation can identify the cause and get you the right treatment.
White Discharge Without Infection
Not all irritation comes from bacteria or fungi.
Atrophic vaginitis
This happens when estrogen drops — most commonly at menopause, after ovary removal, or during certain cancer treatments. Estrogen keeps vaginal tissue thick and moist. Without it, the lining thins, dries out, and tears easily. Moisturizers or topical estrogen help most women. For those avoiding hormones, isoflavone-based gels have outperformed placebos in trials.
Irritant or allergic vaginitis
This is a reaction to something external. The usual culprits: harsh soaps, scented hygiene products, douching, sex toys, latex condoms or diaphragms, sometimes semen. Over-washing is also on this list — it strips protective bacteria and causes tiny tears in the tissue. Plain water is usually enough. Fewer products is almost always better.
White Discharge with Itching or Smell: What It Means
Untreated BV or trichomoniasis raises susceptibility to other STIs, including HIV, herpes, gonorrhea, and chlamydia. In pregnancy, both are linked to preterm labor, low birth weight, and premature rupture of membranes — which is why screening during pregnancy isn’t optional. Untreated BV also raises the risk of complications after procedures like abortion or hysterectomy.
One clinical sign worth knowing about: small red spots on the cervix during an exam are a classic indicator of trichomoniasis. Doctors call it “strawberry cervix.” If a provider mentions it, treatment needs to start immediately.
When Should You See a Gynecologist?
Symptoms alone can’t tell you which infection you have. FOGSI guidelines are explicit: diagnosis requires testing. Your doctor will likely do one or more of:
pH testing — litmus paper or pH-sensitive gloves to check whether your acidity has shifted.
The whiff test — discharge mixed with potassium hydroxide solution. A fishy smell confirms certain bacteria.
Microscopy — looking at cells under a microscope. BV shows “clue cells,” which are vaginal cells coated in bacteria that look fuzzy at the edges. Yeast shows hyphae — branching, thread-like fungal structures.

Self-diagnosis often gets it wrong. A simple test at the clinic can tell you exactly what you are dealing with.
Treatment for White Discharge
All three main infections are treatable.
BV and trichomoniasis respond to metronidazole or tinidazole. Yeast responds to oral fluconazole or topical azole creams.
If you’re prescribed metronidazole: no alcohol for at least 24 hours after your last dose. The combination causes nausea, vomiting, and flushing. It’s not subtle, and it catches people off guard when they don’t know to avoid it.
On partners: BV and yeast don’t usually require treating male partners. Trichomoniasis is different. It’s an STI, and partners need treatment at the same time even without symptoms. If only one person gets treated, the infection just comes back. That “ping-pong” reinfection pattern is why so many cases of trich keep recurring despite treatment.
Probiotics and recurrence
Lactobacillus rhamnosus GR-1 and Lactobacillus fermentum RC-14 are the two strains with the most clinical evidence for vaginal health. Cochrane reviews suggest combining antibiotics with probiotics outperforms antibiotics alone, though probiotics are a support, not a standalone treatment.
Recurrence is defined as an infection returning within 3 to 4 months, or up to 3 to 4 years for chronic patterns. If infections keep coming back, a fuller workup is warranted: PAP smear, HPV screening, vaginal swabs. It’s also worth checking the partner — someone can carry Candida without symptoms, and uncontrolled diabetes in either person makes yeast harder to clear and more likely to return.
Prevention
Wash with plain water or unscented soap. Scented and flavored products don’t belong anywhere near the vagina.
Don’t douche. It disrupts protective bacteria and raises infection risk — this one is well established.
Use condoms, particularly with new or multiple partners.
If you’re pregnant, ask about pH screening. Elevated pH is associated with preterm birth and it’s a simple, cheap thing to check.
If infections keep coming back, Lactobacillus GR-1 and RC-14 supplements are worth trying alongside treatment. The evidence isn’t as strong as for antibiotics, but it exists.

If you are experiencing abnormal white discharge, itching, or discomfort, consult Dr. Pallavi Kulkarni for personalised care.
Women experiencing white discharge problems often consult Dr. Pallavi Kulkarni, gynecologist in Kandivali East, for proper diagnosis and treatment.
Do you have any questions?
Request An AppointmentFAQ
What is normal vaginal discharge and when should you worry?
Normal discharge is clear or white, doesn’t smell strongly, and is thin or slightly sticky. It changes across your cycle — more watery around ovulation, thicker at other times — and that’s normal.
What needs attention: discharge that turns yellow or green, becomes frothy or very thick, smells foul, or comes with itching, burning, redness, or pain. Any one of those is enough reason to get checked.
What causes abnormal vaginal discharge?
Three infections account for most cases — bacterial vaginosis, yeast infection, and trichomoniasis — but irritation from external triggers (soaps, hygiene products, latex condoms, sex toys) can also change discharge without any actual infection. That matters because treatment is completely different depending on which it is.
Can you tell which infection you have from symptoms alone?
Roughly, sometimes. BV tends to cause thin, off-white discharge with a fishy smell, often worse after sex. Yeast usually means thick white discharge with intense itching and redness, but no bad smell. Trichomoniasis can cause foul-smelling, frothy yellow-green discharge with soreness and inflammation.
But these patterns aren’t reliable enough to diagnose yourself. The symptoms overlap. Two infections can coexist. Trichomoniasis in particular gets missed because it can look like BV. A proper examination is the only way to know.
What raises the risk of vaginal infections?
Recent antibiotics are the biggest one — they strip protective bacteria and leave the vaginal environment open to overgrowth. Uncontrolled diabetes, douching, and smoking also raise risk. So do new or multiple sexual partners without condoms, and certain contraceptives including IUDs and regular spermicide use.
External triggers are worth their own look: soaps, tampons, sex toys, latex, diaphragms. If infections keep recurring, something in that list often turns out to be the cause — and it’s usually fixable once identified.
Is white discharge normal?
Yes. Mild white discharge without a strong smell or itching is usually normal. It changes in consistency through your menstrual cycle — thinner around ovulation, thicker at other times. This is your body’s natural way of keeping the vaginal environment clean.
When should I worry about white discharge?
If the discharge is accompanied by itching, a bad smell, a change in colour (yellow, green, grey), pain, or a cottage-cheese-like texture, it could indicate an infection. These symptoms warrant a visit to the gynecologist rather than self-treatment.
Can white discharge be a sign of infection?
Yes. Thick white discharge with itching is often a fungal (yeast) infection. Thin greyish-white discharge with a fishy smell usually points to bacterial vaginosis. The only way to know for sure is through proper testing at a clinic.
When do you need to see a doctor?
If you notice strong odour, unusual colour, itching, burning, soreness, or pelvic pain. Also if the same infection keeps coming back — repeating treatment without investigating why it recurs doesn’t actually solve anything.
Pregnancy makes this more urgent. Untreated BV and trichomoniasis carry real risks, including preterm labour. Don’t wait to see if it clears up. The same applies after any gynaecological procedure. And if you’ve had three or more infections in a year, that’s a pattern worth investigating properly, not just treating each episode and moving on.
