Gynecological Infections Treatment in Kandivali East
Vaginal infections, urinary tract infections, and pelvic infections are some of the most common reasons women visit a gynecologist. They can cause anything from mild itching to persistent pain, and many women put off seeking help because the symptoms feel awkward to discuss.
The good news is that most of these infections respond well to treatment when caught early. At Aarogya Women’s Clinic in Kandivali East, Dr. Pallavi Kulkarni offers a private, comfortable space where you can discuss your symptoms openly and get clear answers about what is going on.

What Are Gynecological Infections?
A gynecological infection is any infection that affects the reproductive or urinary system — the vagina, cervix, uterus, fallopian tubes, or bladder. Bacteria, fungi, viruses, and parasites can all be responsible.
These infections are extremely common. Some cause obvious symptoms like itching, unusual discharge, or pain during urination. Others produce no symptoms at all and are only found during a routine check-up.
When diagnosed early, most gynecological infections clear up with straightforward treatment. Left untreated, though, even a mild infection can spread and lead to more serious problems down the line.
Experiencing unusual discharge, itching, or discomfort? Early diagnosis leads to faster recovery.
Types of Gynecological Infections
The most common types include:
- Vaginal yeast infections (candidiasis) — fungal overgrowth that causes itching, thick white discharge, and irritation. Very common and usually easy to treat.
- Bacterial vaginosis (BV) — happens when the natural balance of vaginal bacteria is disrupted. Typically noticed as a greyish discharge with a fishy odour.
- Urinary tract infections (UTIs) — a burning sensation when you urinate, along with a constant urge to go, are the hallmark signs. UTIs affect the bladder or urethra.
- Pelvic inflammatory disease (PID) — a more serious infection that reaches the uterus, fallopian tubes, or ovaries. Can cause pelvic pain and, if untreated, affect fertility.
- Sexually transmitted infections (STIs) — chlamydia, gonorrhoea, and trichomoniasis can all cause discharge or pain, though many STIs produce no symptoms at all.
Because the causes differ, so does the treatment. Getting the right diagnosis is the first step.
Symptoms Women Should Not Ignore
It is easy to dismiss a mild itch or a slight change in discharge as “nothing serious.” But these are often the first signs that something needs attention. Watch for:
- Vaginal discharge that looks or smells different from what is normal for you
- Itching, irritation, or soreness around the vaginal area
- A burning feeling when you urinate
- Pelvic pain or a dull ache in the lower abdomen
- Discomfort or pain during intercourse
- Needing to urinate frequently or urgently
- Fever or chills along with any of the above
None of these symptoms should be brushed aside. If something feels off, it is worth getting it checked rather than waiting and hoping it goes away on its own.
When to See a Gynecologist for Infections
Many women try to manage symptoms on their own — and for something like a mild yeast infection, that sometimes works. But there are situations where seeing a gynecologist is the better choice:
- Symptoms have lasted more than a few days despite home remedies or pharmacy medication
- Over-the-counter treatment did not help, or the infection came back
- You get the same infection three or more times in a year
- You have fever, chills, or pelvic pain along with other symptoms
- Your discharge is blood-tinged or has a strong, foul smell
- You are pregnant and suspect an infection
Self-medication can sometimes mask the real problem or treat the wrong cause entirely. A proper diagnosis means you get the right treatment the first time.


How Gynecological Infections Are Diagnosed
At Aarogya Women’s Clinic, the first step is understanding what you are experiencing. A typical evaluation includes:
- A conversation about your symptoms, how long they have been present, and any treatments you have already tried
- A clinical examination to look for visible signs of infection
- Vaginal swab tests to identify whether bacteria, fungi, or parasites are involved
- Urine testing if a UTI is suspected
- Blood work when the infection appears to have spread beyond the local area
- An ultrasound scan if pelvic inflammatory disease is a possibility
Not every patient needs every test. What is done depends on your specific symptoms and history.
Not sure what is causing your symptoms? A consultation can give you a clear diagnosis and a straightforward treatment plan.
Treatment Depends on the Cause
What works for one infection will not work for another. A yeast infection needs antifungal medication; giving antibiotics for it would actually make things worse. That is why getting the diagnosis right matters so much.
Here is a general overview of how different infections are treated:
- Bacterial infections (including BV) are treated with antibiotics, either as tablets or a topical cream
- Fungal infections like candidiasis respond to antifungal creams, pessaries, or oral tablets
- Viral infections such as herpes cannot be fully cured, but antiviral medication controls symptoms and reduces flare-ups
- Parasitic infections like trichomoniasis are treated with specific antiparasitic medication
- Pelvic inflammatory disease usually requires a combination of antibiotics. Severe cases sometimes need hospital admission.
One important thing: always complete the full course of medication, even if symptoms improve within a day or two. Stopping early is one of the most common reasons infections come back.
Preventing Recurring Infections
If you keep getting the same infection, that is frustrating — and you are not alone. Recurrent yeast infections and bacterial vaginosis are very common. While you cannot prevent every infection, a few habits make a real difference:
- Use mild, unscented soap for intimate hygiene. Avoid douching — it disrupts the natural vaginal environment.
- Cotton undergarments breathe better than synthetic ones. Try not to stay in tight clothing for long stretches.
- Drink enough water and do not hold urine for too long. Regular urination helps flush bacteria from the urinary tract.
- Finish your full course of medication every time, even when symptoms clear up early.
- Come back for a follow-up visit so we can confirm the infection has actually resolved.
- If you have diabetes or another condition that affects immunity, keeping it well-managed reduces your infection risk.
During your consultation, Dr. Pallavi Kulkarni will look at your history and identify what might be triggering recurrences, so the advice you get is specific to your situation.

Why Timely Treatment Matters
Most gynecological infections are not dangerous when treated promptly. The problems tend to start when infections are ignored or treated incorrectly:
- A vaginal or cervical infection can spread upward to the uterus and fallopian tubes, turning into pelvic inflammatory disease
- PID can cause scarring inside the fallopian tubes, which is one of the treatable causes of difficulty conceiving
- Some women develop chronic pelvic pain that lingers even after the infection itself is cleared
- Infections during pregnancy carry additional risks, including preterm delivery
- Infections that are partially treated tend to come back, and each recurrence can be harder to resolve
None of this is meant to alarm you. The point is simple: getting treated sooner is always better than waiting.
Infection Care at Aarogya Women’s Clinic
We understand that talking about intimate infections can feel uncomfortable. At Aarogya Women’s Clinic, every consultation is completely private, and Dr. Pallavi Kulkarni takes the time to listen without rushing.
Here is what you can expect:
- A private, unhurried consultation where you can describe your symptoms openly
- A thorough examination to pinpoint the cause — not just treat the surface symptoms
- A clear treatment plan explained in plain language, so you know exactly what to do
- Practical advice on preventing the infection from coming back
- A follow-up visit to make sure the treatment worked
Whether this is your first infection or a problem that keeps returning, you will get straightforward answers and a treatment plan that works.

Common Gynecological Infections — Learn More
Want to read more about a specific condition? These pages go deeper into causes, symptoms, and treatment options:
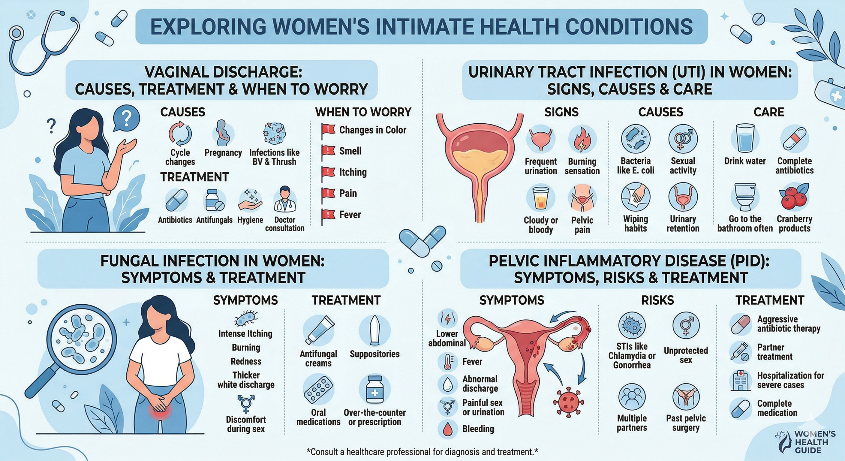
- Vaginal Discharge: Causes, Treatment, and When to Worry — coming soon
- Urinary Tract Infection in Women: Signs, Causes, and Care — coming soon
- Fungal Infection in Women: Symptoms and Treatment — coming soon
- Pelvic Inflammatory Disease: Symptoms, Risks, and Treatment — coming soon
Dealing with symptoms that won’t go away? Do not wait for things to get worse. Dr. Pallavi Kulkarni at Aarogya Women’s Clinic, Kandivali East can help you get the right diagnosis and treatment.
Women across Kandivali West, Borivali East, Borivali West, Malad East, Malad West, Goregaon East, and Thakur Village trust Dr. Pallavi Kulkarni for gynecological infection care.
What Our Patients Say
Do you have any questions?
Request An AppointmentFAQ
What are the most common gynecological infections in women?
Vaginal yeast infections, bacterial vaginosis (BV), urinary tract infections (UTIs), and pelvic inflammatory disease (PID) are the ones seen most often. All of them are treatable, especially when caught early.
Can gynecological infections affect fertility?
They can, yes. Pelvic inflammatory disease in particular can cause scarring in the fallopian tubes, which makes it harder to conceive. This is why treating infections early matters — the risk drops significantly with prompt care.
Is vaginal discharge always a sign of infection?
Not at all. A certain amount of discharge is completely normal and changes throughout your menstrual cycle. What you should pay attention to is discharge that looks different from your usual pattern — especially if it has a strong odour, unusual colour, or comes with itching.
How are gynecological infections diagnosed?
It usually starts with a conversation about your symptoms, followed by a clinical examination. Depending on what is found, the doctor may order vaginal swabs, a urine test, or cultures. An ultrasound is sometimes needed if the infection appears to involve the pelvic organs.
Can gynecological infections recur after treatment?
Unfortunately, yes. Yeast infections and bacterial vaginosis are especially prone to coming back. Antibiotic use, hormonal shifts, and certain lifestyle habits can all play a role. If recurrences are a problem for you, a follow-up consultation can help identify what is triggering them and how to break the cycle.
